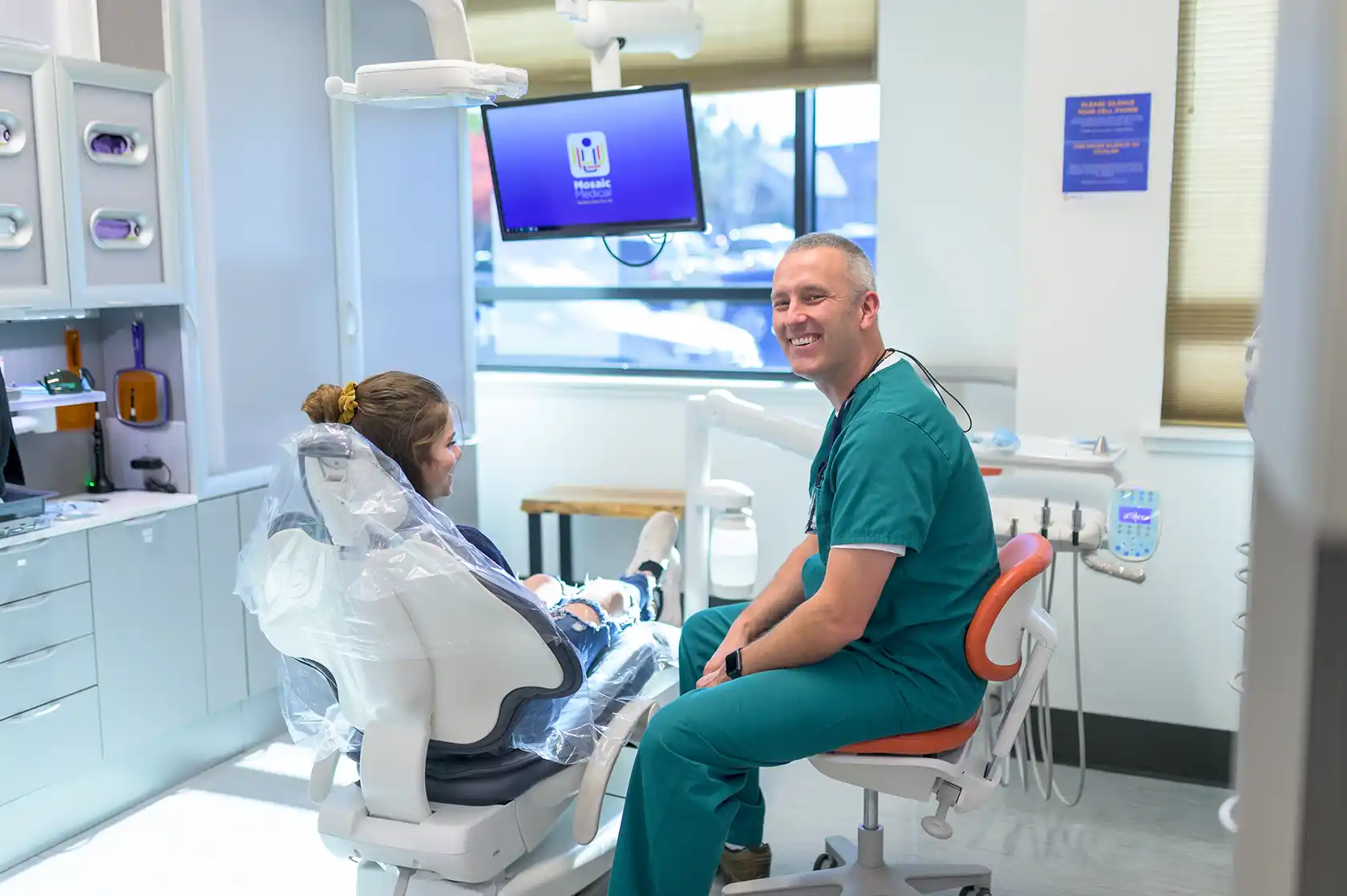
Meet Our Providers
Complete care for all ages
Make an Appointment
Schedule online or call
Find a Location
View health centers near you
Sliding scale discount program
Whether you have insurance or not, you may be eligible for our Sliding Scale discount program and qualify for free or reduced-cost healthcare.
Our Services
Mosaic offers comprehensive services including medical, dental, behavioral health, pharmacy, nutrition and more.
Stories & News

Mosaic Receives $10,000 PacificSource Donation for Inaugural Fundraising Luncheon
Funding Supports “More than Medical” Inaugural Fundraising Luncheon Bend, Oregon, Apr. 18, 2024 – Mosaic Community Health, a nonprofit community health center providing quality care for all in Bend, Redmond, Prineville, Sisters and Madras, has received a $10,000...

Pointers for Parenting a Picky Eater
Are you struggling with parenting a picky eater? This guest blog post from Lindsey Overstreet, LCSW, Behavioral Health Manager at Mosaic provides some great tips for encouraging healthy eating habits in kids. Happy National Nutrition Month! Picky eating is one of the...

Inaugural Event: Mosaic’s “More than Medical” Fundraising Luncheon on May 1, 2024
Guest blog post by Emily Boynton, Senior Development Officer, Mosaic Community Health At Mosaic, we believe that the quality of healthcare should never depend on how much money individuals make, what language they speak, or the status of insurance coverage. We...